Modern clinical medicine and neurobiology research is making revolutionary progress in understanding the somatic reflections of mental processes. Cervical muscle tension, one of the most prominent physical manifestations of psychological stress in the body, can transcend a simple discomfort and become a pathophysiological pressure factor on the Vagus nerve, the fundamental regulator of the autonomic nervous system. This situation triggers a series of reactions that create multisystemic effects throughout the body, particularly by disrupting the biomechanical stability of the Atlas (C1) vertebra. Academic studies on how psychosocial stressors modulate muscle activity, how this activity causes angular deviations in the Atlas vertebra, and how this mechanical deviation disrupts body homeostasis through pressure on the Vagus nerve have brought about a new diagnostic perspective defined as “Cervicovagopathy.”
Pathophysiology of Psychosocial Stress and Cervical Muscle Tension
The relationship between psychosocial stressors, neck pain, and muscle tension is not just a symptom association, but a deep neurophysiological interaction. Stress originating from the workplace or social life has been proven to be an independent variable from physical risk factors in the development of neck pain. While the hypothalamic-pituitary-adrenal (HPA) axis, which is activated during the stress response, increases muscle tone through cortisol and catecholamine release, it has been observed that muscles such as the upper trapezius and sternocleidomastoid (SCM) show selective sensitivity to stressors.
Electromyographic (EMG) analyses reveal a significant increase in activity in the upper trapezius muscle during tasks requiring mental concentration or involving a social evaluation threat, even in the absence of physical movement. This is called the “psychomotor” mechanism. It has been determined that in individuals under stress, muscles cannot fully relax even during rest periods, remaining in a state of low-level but constant activity (sustained muscle activity). Over time, this chronic hypertonicity leads to microtraumas in muscle fibers, oxidative stress, and the formation of trigger points, disrupting the biomechanical balance in the neck and shoulder girdle.
There is a positive correlation between anxiety and depression levels and the severity of neck pain. As the psychological load increases, the individual’s pain perception sharpens, and the defensive guarding mechanism in the muscles becomes permanent. In this process, not only the trapezius muscle but also the suboccipital muscles, which adjust the position of the head millimetrically, are affected.
| Muscle Group | Stress Response and Behavioral Model | Biomechanical Consequences |
|---|---|---|
| Upper Trapezius | Selective activation, increase in resting tone | Elevation of the shoulders, increased load on the cervical spine |
| Sternocleidomastoid (SCM) | Hypertonicity and asymmetric pulling | Rotational restriction of the Atlas and forward head posture |
| Suboccipital Muscles | Continuous isometric contraction, trigger point development | Loss of C1-C2 joint stabilization, Atlas subluxation |
| Scalene Muscles | Overuse due to respiratory stress | Elevation of the first rib and risk of thoracic outlet syndrome |
.
Biomechanical Role and Vulnerability of the Atlas (C1) Vertebra
The Atlas vertebra (C1) is considered the “keystone” of the spinal system. Anatomically distinct from other vertebrae, the Atlas does not have a body (corpus) or an intervertebral disc. Weighing approximately 2 grams, this ring-like bone is responsible for carrying the human skull, which weighs 5-6 kilograms. This enormous weight difference makes the stability of the Atlas extremely dependent on ligaments and the surrounding delicate muscle group.
The atlanto-occipital joint, which the Atlas forms with the skull, provides 30% of the flexion and extension (yes motion) of the head, while the atlanto-axial joint it forms with the Axis (C2) undertakes more than 50% of the rotational capacity (no motion) of the head. This freedom of movement also makes the Atlas the most vulnerable area to external factors and muscle imbalances.
Muscle Tension and Angular Misalignment of the Atlas
Psychological stress-induced muscle hypertonicity creates an asymmetric pulling force on the Atlas vertebra. In particular, the m. obliquus capitis inferior muscle is one of the main muscles controlling the rotation between the Atlas and the Axis. Unilateral tension of this muscle due to stress can cause the Atlas to rotate on the Axis and lock in this position. This condition is defined as “Atlas Blockage” or “Atlas Subluxation Complex” (ASC).
Tension in the SCM muscle also has a critical impact on Atlas biomechanics. The mastoid process, where the SCM attaches to the skull, is very close to the transverse processes of the Atlas. Continuous tension in the SCM restricts the rotational position of the Atlas, causing an asymmetrical load distribution in the joint capsule and leading to the disruption of cervical proprioceptive inputs.
Biomechanical simulations using Finite Element Analysis methods have shown that hypertonicity in the suboccipital muscles can increase the stress on the atlanto-axial joint to
over 37% and disrupt joint stability. This mechanical imbalance not only causes neck pain but also sets the stage for the compression of the neurovascular structures passing in front of the transverse processes of the Atlas.
Anatomical Relationship Between the Vagus Nerve and the Carotid Sheath
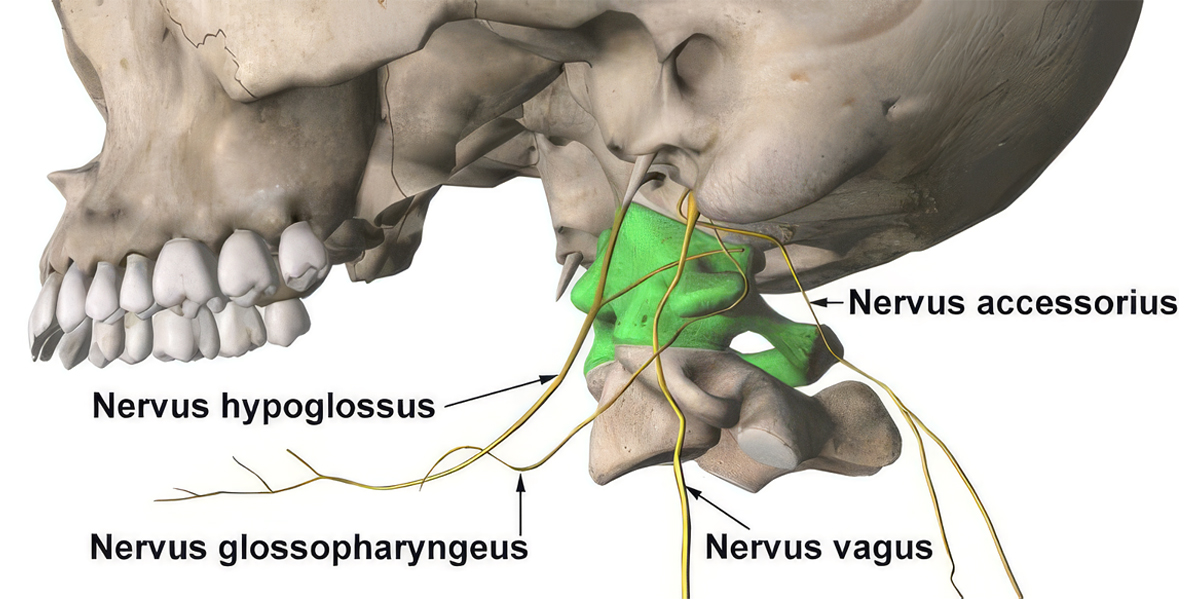
The Vagus nerve (Cranial Nerve X) is the longest and most complex nerve in the body; as its Latin name (“Wanderer”) implies, it exits the brainstem and spreads throughout the neck, chest, and abdominal cavity. The Vagus nerve leaves the cranial cavity via the jugular foramen.
In the neck region, the Vagus nerve is packaged within a tight fascial structure called the “Carotid Sheath,” along with the internal jugular vein (IJV) and internal carotid artery (ICA). This sheath is located directly in front of the transverse processes of the Atlas (C1) vertebra. Any angular deviation in the biomechanical position of the Atlas causes direct pressure to be applied to the structures within this sheath.
Nodose Ganglion: The Critical Control Point
The Nodose Ganglion, which is the inferior ganglion of the Vagus nerve, acts as a sensory hub for the autonomic nervous system. This ganglion is positioned exactly in front of the Atlas (C1) vertebra. Neurons in the nodose ganglion are responsible for transmitting signals to the brain regarding blood pressure, blood oxygen levels, respiratory rate, and stretch signals from the digestive system organs.
When the Atlas vertebra shifts forward or rotates, the transverse process can create direct mechanical irritation on the Nodose ganglion and the Vagus nerve. This mechanical pressure can block blood flow over the nerve fibers (vasa nervorum), leading to ischemic damage or conduction blocks.
Cervicovagopathy: Mechanisms and Stages of Development
“Cervicovagopathy” is a modern clinical term describing the condition where disruptions in the neck structure impair Vagus nerve functions. The primary driver in the development of this condition is the “Modern Lifestyle” (Forward Head-Facedown Lifestyle – FH-FDL) and the chronic stress it brings.
The progression stages of cervicovagopathy can be summarized as follows:
- Initial Stage: Stress, combined with continuous phone and computer usage, causes the posterior cervical ligaments to stretch slowly. The head shifts forward (Forward Head Posture). At this stage, slight stretching and interruptions in electrical conduction begin on the Vagus nerve.
- Progressive Stage: Ligamentous cervical instability develops. The ligaments between the Atlas (C1) and Axis (C2) loosen, causing the Atlas to move uncontrollably and exert pressure on the carotid sheath.
- Advanced Stage: The cervical curve is completely lost (Kyphosis or Military Neck). The Vagus nerve is under continuous stretch and compression. This condition leads to Vagus neuron cell death (degeneration) and permanent autonomic function loss.
Ultrasound studies show that the cross-sectional area (CSA) of the Vagus nerve in these patients is significantly reduced compared to the normal population. Furthermore, it has been documented that the transverse process of the Atlas compresses the internal jugular vein, impairing venous drainage from the brain and indirectly contributing to increased intracranial pressure.
Systemic Effects of Vagus Nerve Compression on the Body
Because the Vagus nerve is the main highway of the parasympathetic nervous system, a disruption here completely overturns the body’s homeostatic balance. When the “Rest and Digest” mechanism, which balances the “Fight or Flight” response, is disabled, the body goes into a constant state of alarm.
Cardiovascular Irregularities and Heart Rate Variability (HRV)
The Vagus nerve slows the heart rate and regulates its rhythm by innervating the SA and AV nodes, the natural pacemakers of the heart. In the case of Atlas-induced Vagus compression:
- Decreased Heart Rate Variability (HRV): HRV is the most sensitive indicator of autonomic nervous system health. Low HRV indicates that the Vagus nerve has lost its ability to modulate the heart and the individual has lost their resilience to stress.
- Tachycardia and Palpitations: Pressure on the nerve weakens the heart’s “brake” mechanism, leading to high heart rates and palpitation attacks even at rest.
- Orthostatic Intolerance (POTS): When the Vagus nerve’s communication with the baroreceptors that regulate blood pressure is disrupted, symptoms such as excessive heart rate increase or dizziness upon standing (POTS) can be triggered.
Gastrointestinal and Metabolic Disorders
The Vagus nerve is the primary controller of stomach acid secretion, digestive enzymes, bile production, and intestinal peristalsis. Common digestive problems seen in cervicovagopathy patients include:
- Gastroesophageal Reflux: The Vagus nerve provides the tone of the lower esophageal sphincter. A dysfunction here causes stomach acid to escape into the esophagus.
- Gastroparesis and Bloating: Chronic bloating, nausea, and indigestion occur as a result of delayed gastric emptying.
- Systemic Inflammation: The Vagus nerve protects the body against inflammation via the “cholinergic anti-inflammatory pathway,” which inhibits cytokine release from macrophages. A drop in vagal tone can lead to low-grade chronic inflammation and trigger autoimmune processes.
Neuropsychiatric Effects and “Brain Fog”
80% of the Vagus nerve consists of sensory (afferent) fibers, which constantly transmit information to the brain about the state of the body. In the event of nerve irritation, erroneous signals sent to the brain lead to the following conditions:
- Brain Fog: When the Atlas vertebra obstructs venous drainage (IJV) combined with Vagus dysfunction; loss of concentration, cognitive slowing, and memory problems are observed.
- Anxiety and Emotional Lability: The Vagus nerve is connected to the limbic system and amygdala in the brain. A drop in vagal signal quality causes the brain to constantly feel unsafe, leading to unprovoked anxiety attacks.
- Sleep Disorders: Autonomic imbalance and pressure on the brainstem make it difficult to fall asleep and reduce the restorative quality of sleep.
Clinical Symptoms and Diagnostic Criteria in the Atlas and Vagus Relationship
Cervicovagopathy and Atlas misalignment conditions often present as “mysterious” or “unexplained” symptom complexes. Patients have frequently visited multiple doctors, yet standard MRIs or blood tests have not revealed significant findings.
The primary biomechanical and neurological parameters used in the diagnostic process are presented in the table below:
| Diagnostic Parameter | Ideal / Normal Value | Pathological Findings | Clinical Correlation |
|---|---|---|---|
| Vagus CSA (Ultrasound) | 2.0 – 3.0 mm² | < 1.5 mm² | Vagus nerve degeneration and neuron loss |
| Cervical Curve Depth | 7 – 17 mm | < 0 mm (Kyphosis) | Excessive stretching in nerve and vascular structures |
| C1-C2 Facet Overhang | < 1 mm displacement | > 2 mm overhang | Atlanto-axial instability and Vagus compression |
| IJV Cross-Sectional Area (at C1) | Patent and wide | Stenosis or collapse | Venous outflow obstruction from the brain, headache, tinnitus |
| Heart Rate Variability (HRV) | High HRV | Low HRV / Low RMSSD | Inability of the autonomic system to adapt to stress |
In the physical examination, tenderness over the Atlas transverse processes, trigger points in the SCM muscle, weakness of the gag reflex, or uvula deviation can provide clues to Vagus nerve damage.
Polyvagal Theory and the Psychophysiological Integrity of the Upper Cervical Region
The Polyvagal Theory, introduced by Stephen Porges, argues that the Vagus nerve is not just a nerve but an evolutionary safety system. According to this theory, the Vagus consists of two parts:
- Ventral Vagal Complex (VVC): Evolutionarily newer and manages the “Social Engagement System.” It is associated with facial expression, tone of voice, and self-soothing.
- Dorsal Vagal Complex (DVC): Older and manages the “freeze” or fainting response in situations of extreme threat.
The nuclei of the VVC are located in the brainstem, in the region right above the Atlas vertebra. The angular displacement of the Atlas and stress-induced muscle tension can cause this modern social engagement system to “short-circuit.” As a result, the individual becomes unable to perceive social safety signals in their environment and becomes biologically trapped in “defense mode.” This condition is a cycle that explains why chronic stress is not just an emotion, but also why it disrupts the neck structure, and why the deterioration in the neck structure makes stress management impossible.
Complications and Associated Syndromes
Atlas misalignment and Vagus compression, rather than being a standalone disease, can be the hidden trigger for many chronic syndromes.
- Mast Cell Activation Syndrome (MCAS): The Vagus nerve controls the stability of immune system cells (mast cells). When vagal signals are disrupted, mast cells can uncontrollably release histamine, leading to allergy-like reactions, skin rashes, and chronic inflammation.
- Atopic Dermatitis and the Itch Cycle: Cases have been documented where the release of cervical muscle tension has improved moderate-to-severe atopic dermatitis symptoms by reducing psychological stress.
- Meniere-Like Symptoms and Tinnitus: Tension of the SCM muscle at the mastoid process and the indirect connections of the Vagus with the auditory system can cause ringing in the ears (tinnitus) and balance issues.
- Eagle Syndrome and Jugular Compression: In some cases, the distance between the Atlas transverse process and the styloid process narrows so much that the IJV and the Vagus nerve become trapped, as if caught between a pair of scissors.
Biomechanical Restoration and Treatment Approaches
The treatment of this complex picture must target structural and neurological restoration rather than merely being symptomatic.
- Atlas Correction: Restoring the normal biomechanical position of the Atlas using manual therapy or special devices (like Spineliner) lifts the compression on the Vagus and the pressure on the IJV.
- Ligamentous Stabilization (Prolotherapy): If ligament laxity (LCI) underlies the Atlas misalignment, strengthening the ligaments with regenerative injections (Prolotherapy) provides lasting stability.
- Muscle Relaxation and Posture Education: Resolving trigger points in the SCM and suboccipital muscles with passive and active techniques stops the asymmetric pulling on the Atlas.
- Vagus Nerve Stimulation (VNS): In addition to manual therapy, transcutaneous VNS applied from the cymba conchae region of the ear sends “safety” signals to the brain, helping autonomic balance to be established more quickly.
- Psychological Support and Stress Management: Cognitive behavioral therapies and relaxation exercises to break the effect of stress on muscle tone must be an integral part of the treatment.
Conclusion
The reflection of psychological stress on the cervical muscles is more than just simple muscle fatigue; it is a process that leads to the biomechanical locking of the Atlas (C1) vertebra, the most strategic point of the spine. This angular misalignment in the Atlas vertebra mechanically restricts both the sensory and motor functions of the Vagus, the body’s most vital nerve. This clinical picture, called “Cervicovagopathy,” causes systemic disorders on a broad spectrum ranging from heart rate to digestion, and from emotional balance to the immune system.
In modern medical practices, examining the upper cervical region in patients with unexplained symptoms such as palpitations, digestive problems, anxiety, and “brain fog” offers the opportunity to treat not just the symptoms, but the root cause of the disease. The biomechanical alignment of the Atlas and the removal of pressure on the Vagus nerve restores autonomic homeostasis by re-engaging the body’s own self-healing mechanisms (parasympathetic activity). Research clearly reveals that cervical structural stability and Vagus nerve health are among the most critical factors determining an individual’s biological resilience to stress.
Yiğit Alp Şimşek
Physiotherapist
Cited Studies
- Cervicovagopathy: ligamentous cervical instability and dysstructure as a potential etiology for vagus nerve dysfunction in the cause of human symptoms and diseases – PubMed
https://pubmed.ncbi.nlm.nih.gov/40672458/ - Cervicovagopathy: ligamentous cervical instability and dysstructure …
https://pmc.ncbi.nlm.nih.gov/articles/PMC12263383/ - Cervicovagopathy: ligamentous cervical instability and dysstructure as a potential etiology for vagus nerve dysfunction in the cause of human symptoms and diseases – Caring Medical
https://caringmedical.com/prolotherapy-news/cervicovagopathy-ligamentous-cervical-instability-and-dysstructure-as-a-potential-etiology-for-vagus-nerve-dysfunction-in-the-cause-of-human-symptoms-and-diseases/ - Differential effects of mental concentration and acute psychosocial stress on cervical muscle activity and posture – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC4968934/ - Stress management as an adjunct to physical therapy for chronic neck pain – PubMed – NIH
https://pubmed.ncbi.nlm.nih.gov/22700538/ - The effect of suboccipital muscle dysfunction on the biomechanics of …
https://pmc.ncbi.nlm.nih.gov/articles/PMC11110322/ - The Association Between Neck Pain and Psychological Distress Experienced by King Abdulaziz University Students: A Cross-Sectional Study – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC10066660/ - Why the Atlas and Axis Matter More Than Most People Realize | UC Spine Care
https://ucspinecare.com/blog/post/why-the-atlas-and-axis-matter-more-than-most-people-realize - Suboccipital Muscles: What They Are and How to Relieve Tension | Iron Neck
https://www.iron-neck.com/blogs/articles/what-are-suboccipital-muscles-and-how-to-relieve-tension-relief - The Importance of the Atlas (C1) and Axis (C2) Vertebrae: Your Body’s Foundation for Health – Krieg Chiropractic Center
https://kriegchiropractic.com/the-importance-of-the-atlas-c1-and-axis-c2-vertebrae-your-bodys-foundation-for-health/ - How Misalignment of the C1 Vertebra Can Trigger Headaches and Neck Pain — And How Manual Therapy Can Help
https://www.healingartspt.net/single-post/how-misalignment-of-the-c1-vertebra-can-trigger-headaches-and-neck-pain-and-how-manual-therapy-can - Atlas joint instability: Causes, consequences and solutions – MSK Neurology
https://mskneurology.com/atlas-joint-instability-causes-consequences-solutions/ - C1-C2 Segment & Upper Neck Dysfunction Overview – Chiropractic & Physiotherapy
https://www.mychiro.com.my/articles/c1-c2-segment-dysfunction/ - The Suboccipitals: Small Muscles, Big Impact – ABMP
https://www.abmp.com/Massage-and-Bodywork-Magazine/Issues/januaryfebruary-2024/suboccipitals-small-muscles-big-impact - Atlas Subluxation Complex, National Upper Cervical Chiropractic …
https://pmc.ncbi.nlm.nih.gov/articles/PMC11927947/ - Neuroimaging features of right IJVS induced by the C1 transverse mass…. – ResearchGate
https://www.researchgate.net/figure/Neuroimaging-features-of-right-IJVS-induced-by-the-C1-transverse-mass-Sagittal-A_fig1_333328160 - Functional anatomy of the vagus system – emphasis on the somato-visceral interface – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC8627476/ - Vagus nerve compression in the neck: Symptoms and treatments – Caring Medical
https://caringmedical.com/prolotherapy-news/vagus-nerve-compression-cervical-spine/ - Microsurgical Anatomy of the Jugular Foramen Applied to Surgery of Glomus Jugulare via Craniocervical Approach – Frontiers
https://www.frontiersin.org/journals/surgery/articles/10.3389/fsurg.2020.00027/full - Anatomical study of jugular foramen in the neck – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC9422587/ - Anatomical Reasons for an Impaired Internal Jugular Flow – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC12472027/ - Cervicovagopathy: ligamentous cervical instability and dysstructure as a potential etiology for vagus nerve dysfunction in the cause of human symptoms and diseases – Frontiers
https://www.frontiersin.org/journals/neurology/articles/10.3389/fneur.2025.1572863/full - Objective test findings in patients with chronic eye symptoms seeking care at an outpatient neck center: ligamentous cervical instability etiology? – Frontiers
https://www.frontiersin.org/journals/neurology/articles/10.3389/fneur.2025.1576315/full - Cervical Instability and Vagus Nerve Symptoms Secrets Revealed: What Oklahoma Doctors Don’t Want You to Know About Prolotherapy and Ozone | Venturis Clinic
https://venturisclinic.com/regenerative-medicine-blog/cervical-instability-and-vagus-nerve-symptoms-secrets-revealed-what-oklahoma-doctors-dont-want-you-to-know-about-prolotherapy-and-ozone/ - The ligamentous cervical instability etiology of human disease from …
https://pmc.ncbi.nlm.nih.gov/articles/PMC11638589/ - Cervical Oculopathy: The Cervical Spine Etiology of Visual Symptoms and Eye Diseases—A Hypothesis Exploring Mechanisms Linking the Neck and the Eye – ResearchGate
https://www.researchgate.net/publication/396757154_Cervical_Oculopathy_The_Cervical_Spine_Etiology_of_Visual_Symptoms_and_Eye_Diseases-A_Hypothesis_Exploring_Mechanisms_Linking_the_Neck_and_the_Eye - Characterizing Initial Cervical Spine and Neurovascular Findings in 84 Consecutive Patients with Hypermobile Ehlers–Danlos Syndrome: A Retrospective Study – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC13026537/ - What Every Chiropractor Should Know About Vagal Tone and Heart Rate Variability
https://insightcla.com/blog/chiropractic-vagal-tone-heart-rate-variability/ - The Vagus Nerve – Polyvagal Institute
https://www.polyvagalinstitute.org/vagusnerve - The vagus nerve and HRV: How to unlock your parasympathetic superpower – Ultrahuman
https://blog.ultrahuman.com/blog/the-vagus-nerve-and-hrv/ - The Basics Polyvagal Theory and Chiropractic – Prior Lake Spinal Care
https://www.priorlakespinalcare.com/the-basics-polyvagal-theory-as-it-relates-to-chiropractic/ - Can cervical spine instability cause cardiovascular-like symptoms including atrial fibrillation, heart palpitations and blood pressure problems? – Caring Medical
https://caringmedical.com/prolotherapy-news/hrv/ - Are changes in pain associated with changes in heart rate variability in patients treated for recurrent or persistent neck pain? – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC9531383/ - Effects of Chinese cervical fixed-point rotation manipulation on heart rate variability in patients with sympathetic cervical spondylosis based on the theory of biomechanical equilibrium: a study protocol for a randomized controlled trial – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC12510945/ - Mast cell activation syndrome, neck pain and the vagus nerve – Caring Medical
https://caringmedical.com/prolotherapy-news/mast-cell-activation-syndrome/ - An Overview of Vascular Compression Syndromes and Associations with Autonomic Dysfunction: A Review – MDPI
https://www.mdpi.com/2227-9059/14/3/689 - Polyvagal Theory: A Science of Safety – PMC – NIH
https://pmc.ncbi.nlm.nih.gov/articles/PMC9131189/ - Integration of External Vagus Nerve Stimulation in the Physiotherapeutic Management of Chronic Cervicogenic Headache: A Case Report – MDPI
https://www.mdpi.com/2227-9032/13/16/2030 - Compression of the brainstem – Atlantoaxial instability and Atlas displacement
https://caringmedical.com/prolotherapy-news/upper-cervical-instability-affects-brain-stem/ - Traumatic Atlanto-Occipital Dislocation Presenting With Dysphagia as the Chief Complaint: A Case Report – KoreaMed Synapse
https://synapse.koreamed.org/func/download.php?path=L2hvbWUvdmlydHVhbC9rYW1qZS9zeW5hcHNlL3VwbG9hZC9TeW5hcHNlWE1MLzEwNDFhcm0vcGRmL2FybS0zNy00MzgucGRm&filename=YXJtLTM3LTQzOC5wZGY= - Polyvagal theory: a journey from physiological observation to neural innervation and clinical insight – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC12479538/ - The vagus nerve: a cornerstone for mental health and performance optimization in recreation and elite sports – Frontiers
https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2025.1639866/full - Release of Cervical Muscle Tension Improves Psychological Stress and Symptoms of Moderate-to-Severe Atopic Dermatitis: a Case Series with 20 Patients – PMC
https://pmc.ncbi.nlm.nih.gov/articles/PMC9515250/ - Release of Cervical Muscle Tension Improves Psychological Stress and Symptoms of Moderate-to-Severe Atopic Dermatitis: a Case Series with 20 Patients – PubMed
https://pubmed.ncbi.nlm.nih.gov/36129669/